
Are YOU eating too much SUGAR?😱
End the sugar-coating

Added sugar is bad for us and health advice tells us we should limit the amount we eat. But food producers aren’t required to label it. And to make matters worse, sugar is hidden in ‘healthy’ foods such as energy bars and fruit and oat clusters too – not just processed junk foods like confectionery and soft drinks.
Many Australians are over-consuming added sugar, but may not even realise it. It’s clear that this situation needs to change.
In this article:
- What are added sugars?
- Added sugar in ‘health’ foods
- What’s really inside the pack?
- CHOICE calls for better labelling
- How to avoid added sugars
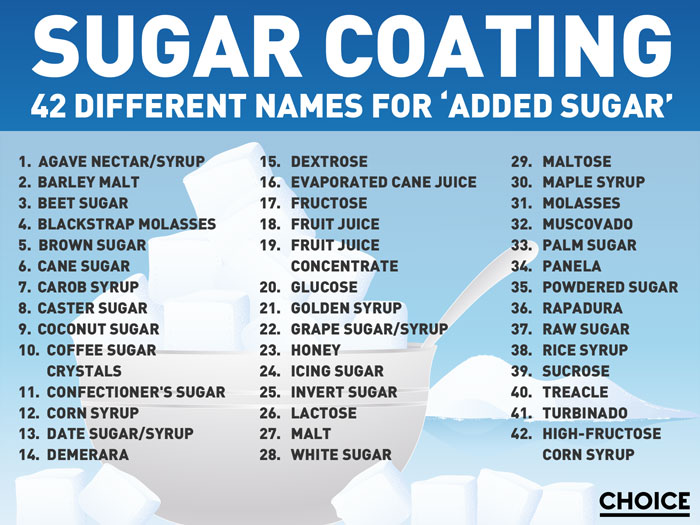
- 40+ different names for added sugars
Sugary ‘health’ foods
While on the hunt for a healthy snack at the supermarket, many people would reasonably head to the health food aisle. You know the one – the aisle with all the products claiming to be ‘gluten free’, ‘natural’ or ‘organic’.
What you might not expect to find are so-called healthy products laden with sugar. But we found substantial amounts of added sugar in products presented as good-for-you – in the health food aisle and elsewhere – and in some cases it took some serious sleuthing to determine that this was the case.
- Clif Chocolate Chip Bar, located with other sports and protein supplements, provides ‘nutrition for sustained energy’, but is also 32% sugar in a number of guises including brown rice syrup, cane syrup and barley malt extract.
- Go Natural Twisters Fruit Snack, which we found in the health food aisle, claims to be gluten and additive free. The brand name implies that they’re ‘natural’, but they’re 67% sugars in the form of concentrated apple puree and juice as well as concentrated strawberry juice.
- Uncle Tobys Plus, Peach, Sultanas and Oat Clusters may be “high in wholegrain” and provide “20% of your daily protein”, but there’s no getting away from the fact that its ingredients include multiple added sugars (sugar, invert sugar, malt extract, glucose solids, golden syrup, and honey to name a few), which make up the bulk of its 23% total sugars.
- Weight Watchers Coconut Delight bars are an approved snack under the Weight Watchers weight loss program, but are 37% sugar with invert sugar, barley malt extract and honey all contributing to this total.
A look inside the pack
We analysed the ingredients list and nutrition information panel of some of the foods we found in the health food aisle to show just how much added sugar – compared with other ingredients – they contain.
Go Natural Berry Frugo’s
On the pack: “Goodness tastes better”, “All natural”, “Source of calcium”, “Gluten free”, “No artificial colours, flavours or preservatives”.
In the pack:
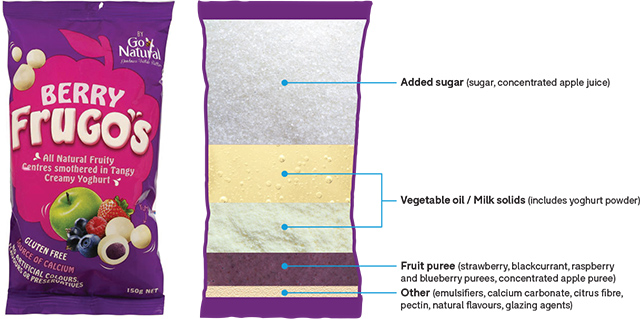
Golden Days Apricot Delight
On the pack: “Natural choice”, “Made with real fruit”, “Gluten free”, “Dairy free”, “No artificial colours”, “No artificial flavours”.
In the pack:

Lowan Cocoa Bombs
On the pack: “Gluten free”, “Low fat”, “No artificial flavours”.
In the pack:

The problem with food labels
Currently there’s no clear way of knowing how much sugar has been added to a food by looking at the label.
You can check the ingredients list to see if a product contains added sugar – the higher up the list, the more sugar the product contains. But added sugars can be disguised under 42 different names and distributed throughout the ingredient list, so they’re not always straightforward to identify and even harder to quantify.
You can also look to the amount of total sugar in a product on the Nutrition Information Panel (NIP). However, this total doesn’t differentiate sugars that have been added by the manufacturer (including glucose, honey and fruit juice concentrates) from those that are intrinsic to the food or one of its ingredients (such as lactose in milk). See What are added sugars for more.
But neither of these labelling elements helps people to easily determine what and how much added sugar is in their food. With so many terms disguising added sugar, and total sugar information sending mixed health messages, it’s evident that current labels are failing consumers.
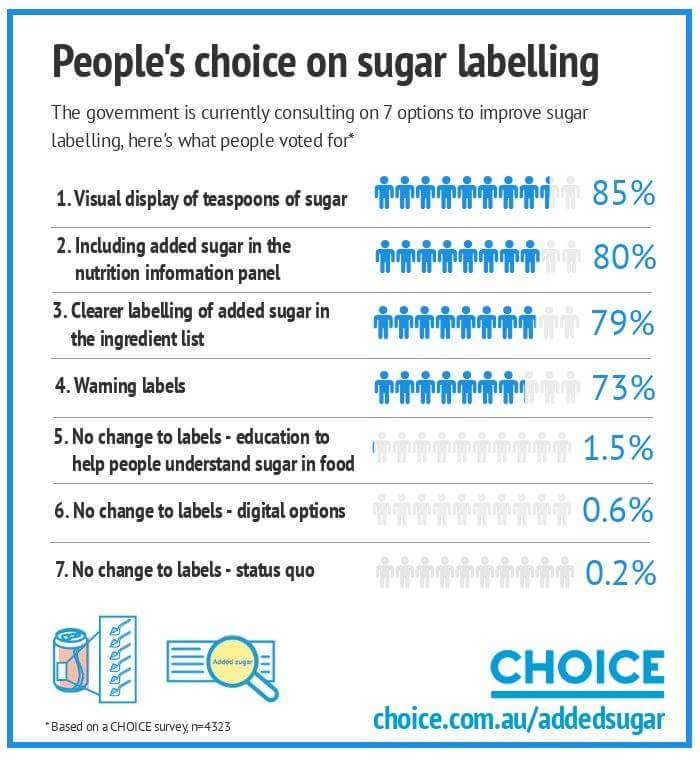
CHOICE calls for better labelling
We need clear and meaningful added sugar labelling so that we can follow advice to limit added sugar consumption and maintain a healthy diet. There are three main changes we want to see:
- Show the number of teaspoons of sugar in sugar-sweetened drinks. Soft drinks and other sugar-sweetened beverages are the number one contributor to our added sugar intake. Some teenagers are consuming 38 teaspoons of added sugar a day, equivalent to the sugar in four cans of Coke. Identifying the amount of teaspoons of sugar on these products would clearly indicate just how much sugar they contain.
- Make it easy to spot added sugar in the ingredients list. Food companies use over 40 different words for added sugar, including muscovado, rapadura or barley malt extract. We want all added sugar ingredients to be grouped together in the ingredient list so that people can clearly identify them.
- Include added sugar in the nutrition information panel. Currently the nutrition information panel (NIP) only displays total sugars, which includes both intrinsic and added sugar. Intrinsic sugars are found in nutrient-rich foods such as milk, fruit and vegies. These foods are recommended by our dietary guidelines and are part of a healthy and balanced diet. The advice is to reduce the intake of added sugar, which is the sugar added to a product by the food manufacturer. This is why we want the amount of added sugar to be identified separately on the NIP.
The government is currently consulting on improvements to sugar labelling. To have your say on what changes you’d like to see, join our campaign.
How to avoid added sugars
The majority of the sugar we eat comes from processed foods. So labelled or not, the most effective way to curb your added sugar intake (and at the same time improve the nutritional quality of your diet) is to eat a wide variety of fresh fruit, vegetables and other whole foods and minimise the amount of processed foods you eat.
Added sugar FAQs
Different names for added sugar
https://www.choice.com.au/food-and-drink/nutrition/sugar/articles/added-sugar
Do you KNOW how much SUGAR your really eating?🤔
Find out how can YOU IMPROVE your ability to tolerate ALLERGENS and reduce allergic reactivity.🤧🍃

The Immune System in Overdrive
Allergy is essentially a state of immune hyper-reactivity. The body encounters an allergen (a foreign substance such as dust, animal fur, pollen, certain food) that triggers a reaction. In an attempt to restore balance, the immune system mounts an attack to eradicate the allergen. This typically involves mast cells releasing histamine and other immune factors, causing an explosion of inflammation – the end result being uncomfortable allergic symptoms.
While meant to be short-lived, the immune response can continue and become chronic. This may be due to the persistence of the allergen in the environment or the diet (perhaps unidentified), or because the immune system remains in a state of hyper-reactivity as other imbalances in the body (e.g. digestive and immune dysregulation) perpetuate the allergic response.

Building up Tolerance to Your Allergenic Enemies
Many seek relief from allergic symptoms, but how? Allergen avoidance can be restrictive, is not always practical, and fails to address the causes of immune imbalance. While natural medicines with antihistamine and anti-inflammatory properties such as Aller-7® herbal combination, quercetin and bromelain can provide much needed relief from the intensity of allergic symptoms, the real answer is in addressing the immune dysregulation that lies beneath the surface. This approach focuses on increasing tolerance – so you essentially become more accepting of the very allergens you react to!
Building up greater tolerance to environmental and food-borne substances dampens down the immune response, ultimately resulting in no or low reaction upon exposure – to ultimately break the cycle of recurrent allergies.
Reducing Allergic Reactivity
The following treatment strategies can improve your ability to tolerate allergens and reduce allergic reactivity through addressing the underlying drivers:
- Restore immune balance: Allergies reflect a dysregulated immune system; a key treatment target. The medicinal mushroom reishi is effective at restoring the balance of immune cells (T helper 1/T helper 2) to a less allergic state.1,2
- Enhance muscosal defences: Secretory immunoglobulin A (an immune factor found in mucus) helps stop allergens in their tracks, providing the first line of defence against the external environment.3,4 These actions are also enhanced by shiitake mushroom.5
- Heal the gut: The digestive system is the body’s prime regulator of immunity, and research shows that people with allergies have greater intestinal permeability6 (which can allow allergens to pass from the gut to the systemic circulation to trigger immune reactivity). Healing the gut lining can promote a strong barrier and reduce allergy.
- Moderate the gut microbiome: Probiotics support a healthy gut microbiome, meanwhile having profound effects on tipping immune balance from reactivity to a state of calm. In particular, Lactobacillus rhamnosus (LGG®)7 and Lactobacillus paracasei LP-33®8 help regulate the immune system and promote an anti-inflammatory environment; also reducing allergic symptoms including eye symptoms9 and eczema.10
- Support detoxification: Liver detoxification aids removal of environmental toxins and food-based allergens,11 as well as immunologically active material from the body, reducing the intensity of the immune reaction.12
A Fresh Approach to Allergy
It’s time to look at allergies from a fresh perspective. In addition to symptomatic support, addressing gut and immune dysregulation as causative factors in allergy allows you to build up your immune tolerance – decreasing the frequency and/or intensity of your allergies to greatly improve how you feel and function.
For more information on Allergy, plug in your headphones and listen to the Allergy Series podcasts.
References
1. Powell M. The use of Ganoderma lucidum (Reishi) in the management of histamine-mediated allergic responses. Townsend Letter: The Examiner of Alternative Medicine. 2006 May 1(274):78-82.
2. Chang H-M, But P P-H. Lingzhi. Pharmacology and applications of Chinese materia medica Vol 1. Singapore; World Scientific Publishing Co. Pte. Ltd. 2001. 1986. p. 598.
3. Mantis NJ, Rol N, Corthésy B. Secretory IgA’s complex roles in immunity and mucosal homeostasis in the gut. Mucosal Immunol. 2011 Nov 1;4(6):603-11.
4. Corthësy B. Secretory immunoglobulin A: well beyond immune exclusion at mucosal surfaces. Immunopharmacol immunotoxicol. 2009 Jun 1;31(2):174-9.
5. Dai X, Stanilka JM, Rowe CA, Esteves EA, Nieves C Jr, Spaiser SJ, et al. Consuming Lentinula edodes (Shiitake) mushrooms daily improves human immunity: a randomized dietary intervention in healthy young adults. J Am Coll Nutr. 2015;34(6):478-87.
6. Miller A. The pathogenesis, clinical implications and treatment of intestinal hyperpermeability. Alt Med Rev [Internet]. 1997 [cited 2017 Jul 13]. Available at: http://static1.1.sqspcdn.com/static/f/290061/15262306/1322064750827/Intestinal_Hyperpermeability.pdf?token=0vEeWSqCFTx9k6wiH6hvN17fXc8%3D.
7. Fong FLY, Kirjavainen PV, El-Nezami H. Immunomodulatory effects of Lactobacillus rhamnosus GG on dendritic cells, macrophages and monocytes from healthy donors. Journal of Functional Foods. 2015;13:71-79.
8. Peng G, Hsu C. The efficacy and safety of heat-killed Lactobacillus paracasei for treatment of perennial allergic rhinitis induced by house-dust mite. Paediatric Allergy and Immunology. 2005;16:433-438.
9. Peng G, Hsu C. The efficacy and safety of heat-killed Lactobacillus paracasei for treatment of perennial allergic rhinitis induced by house-dust mite. Paediatric Allergy and Immunology. 2005;16:433-438.
10. Kalliomäki M, Salminen S, Poussa T, Isolauri E. Probiotics during the first 7 years of life: a cumulative risk reduction of eczema in a randomized, placebo-controlled trial. J Allergy Clin Immunol. 2007;119:10169-1021.
11. Gao B, Jeong WI, Tian Z. Liver: an organ with predominant innate immunity. Hepatology. 2008 Feb 1;47(2):729-36.
12. Mills S, Bone K. Herbal approaches to system dysfunctions. Principles and Practice of Phytotherapy. 2nd edition. Edinburgh: Churchill Livingstone. 2013. p. 198-199.
Aller-7® is a registered trademark of Network Nutrition.
Check out the latest ‘WELLNESS REVIEW- HORMONE HARMONY”.🍃🌸





![]()
This is what goes on inside the body when we are chronically stressed
How stress affects your body – Sharon Horesh Bergquist
Let’s Begin…

If this is you… it’s time to get some help!😱😴
Turmeric! Are you taking an effective dose?🤔🍃
Nature’s Cure-Alls
In the late 1950s and 60s, it was not uncommon for a daily dose of foul-tasting, fishy smelling liquid to be forced upon sickly children by their grandparents and cited as the cure for everything from arthritis and baldness, to boils and piles. Cod liver oil consumption was at its peak, simultaneously torturing yet improving the health of children and their families all over the world. In the decades that followed various other natural remedies came in and out of the limelight. Apricot seed kernels, goji berries and coconut oil all enjoyed their glory days – with some developing a near cult following. However, as time passed and science accumulated (or failed to accumulate), it became clear that these natural remedies weren’t really the ‘cure all’ they were sometimes promoted to be. In recent years, another natural medicine has forged ahead as the latest trendy cure-all taking the population by storm; yet this one has the scientific backing to boot.
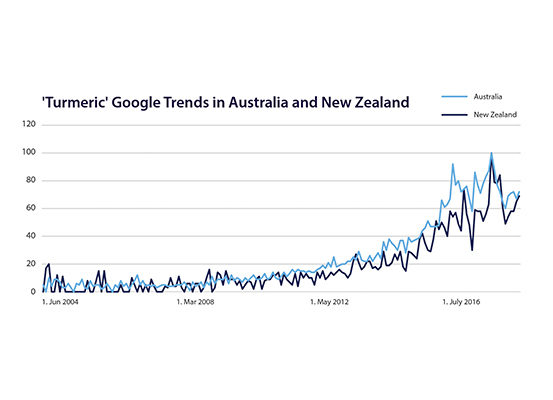
Figure 1a. Turmeric is Trending Amongst Consumers. Google Trends Showing the Public Interest in ‘Turmeric’ in Australia and New Zealand.
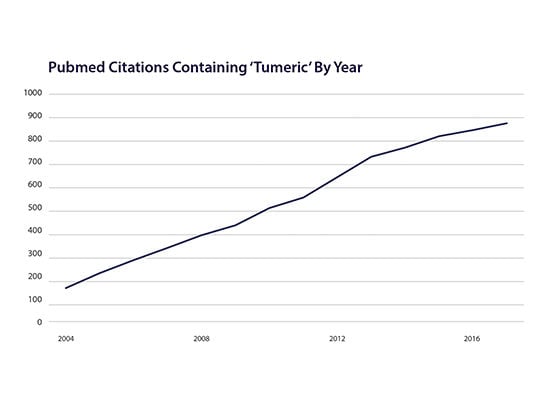
Figure 1b. Turmeric is Trending in Research. PubMed Citations Containing ‘Turmeric’ by Year.
A Condiment and a Cure
The cultural and medicinal history that surrounds turmeric is one that transcends time. Used for at least 6000 years in traditional medicine, food preparation and religious practice, it was long considered to be a sacred harbinger of prosperity amongst many Indian communities. Today, a cascade of promising studies have verified the value it brings. Developing a strong reputation as an anti-inflammatory and antioxidant early on, turmeric now boasts over 7500 scientific publications, which show it benefits a huge array of health conditions: arthritis1,2 cardiovascular disease,3 Alzheimer’s disease4 improved oral hygiene;5 it even has anti-ageing properties. You name the ailment, there is a good chance turmeric has been indicated to be of benefit – and that what you’ve heard is true. Unsurprisingly, all of these emerging health applications have roused a huge love affair with turmeric which has seen turmeric supplements prosper commercially, almost doubling sales within a year.6 However, like all great love affairs it is not without some challenges, and emotional baggage.
Curcumin – Just One Part of a Whole
First isolated in 1815, curcumin, the constituent that gives turmeric its yellow colour, takes much of the credit for the overall benefits of turmeric. This has led to the influx of several isolated curcumin supplements onto the natural medicines market. However, as the wise Greek philosopher Aristotle once proclaimed, the benefits of the whole herb is much greater than the sum of its parts, or more specifically, than one part alone. Certainly, curcumin is a gifted compound however, the whole turmeric root also provides resins and other volatile oils such as turmerones which offer additive anti-inflammatory,7 antimicrobial8 and anticancer9 effects. The first challenge when selecting the most appropriate turmeric supplement to engage in a relationship with, is to ensure you opt for the whole herb (i.e. the label reads Curcuma longa – Turmeric) to achieve the best outcomes; as using curcumin alone limits its therapeutic potential.
Turmeric’s Emotional Baggage
What many don’t realise is, regardless of whether you select the whole turmeric or curcumin alone, another major relationship conundrum remains: the compound curcumin (which comes with both) has notoriously poor bioavailability, meaning, it has low absorption and uptake into the body (aka the emotional baggage) (Figure 2).10 In fact, several animal studies have shown that as much as 90% of oral curcumin is excreted (from the other end). Drinking your daily turmeric latte and having the occasional Indian takeaway, therefore, could be giving you a false sense of security – that you’re obtaining all the potential health gains from this extraordinary herb, however you may not actually be absorbing sufficient levels. Turmeric supplements help overcome this relationship hurdle by providing concentrated extracts, which far exceed even the most impressive dietary intakes of curry. That said, absorption issues still need to be addressed, something that every manufacturer of Turmeric supplements is aware of.
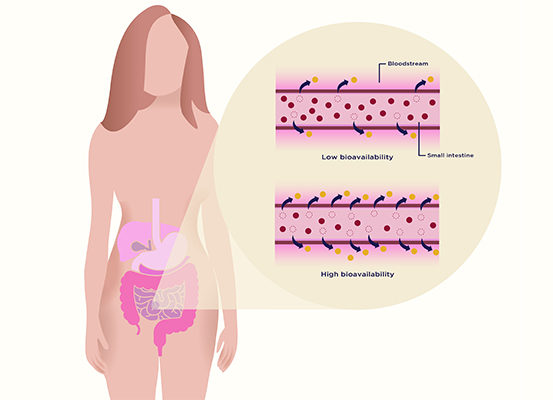
Figure 2: Bioavailability Refers to How Well Something Can be Absorbed and Used by Your Body.
The Turmeric Arm’s Race
In response to the analyses proving poor turmeric absorption, a competitive buzz has been generated amongst supplement manufacturers who strive to meet the challenges of this talented yet temperamental therapy. Hi-tech, impressive-sounding bioavailability technologies such as nanoparticles, liposomes, micelles and phospholipid complexes – anything which can get it out of the intestines and into the blood as efficiently as possible – are constantly being evaluated and promoted to health professionals and consumers alike.11 Fortunately, the whole herb does enhance curcumin absorption thanks to the addition of the volatile oils. Many of the other options are heavily reliant on additives to perform, and as one tablet can only fit so many ingredients before it becomes a ‘horse-pill’, this often comes at the expense of the curcumin content itself. It is also very difficult to evaluate which technology is the leader in this turmeric arm’s race. Head-to-head studies directly comparing the different technologies are sparse, and they use different methodologies to assess absorption – so for the most part it can be like comparing apples with oranges. To throw another spanner in the works, the latest science on turmeric is showing that while bioavailability is likely important, it may not be the sole or even primary factor that determines its effectiveness. That’s because the time turmeric spends in the digestive tract contributes to its health benefits across all systems of the body – including the joints, heart and brain.
Health Begins in the Gut
Perhaps the single most recited quote amongst natural medicine circles is that from Hippocrates: “all disease begins in the gut.” Sharing this wisdom over 2000 years ago, we now have scientific confidence that truer words have never been spoken. The surface area of the inner lining of the digestive tract is thought to be roughly the size of a studio apartment12 – and even though it technically sits inside of our body, it acts as the primary interface with our outside environment. Not only is it a direct physical barrier protecting against entry from the constant assault of inflammatory toxins, dietary antigens, and microbes (like bacteria), it houses more nerves than the rest of our nervous system put together, and directs more immune decisions in one day than the entire immune system makes in a lifetime. In addition to this impressive resume, it is also home to a more than a 90% share of the human microbiome (the microbes that live on us and in us) – which in the last decade has proven to be intimately connected with all aspects of human health.
It comes as no surprise that weakening of the gut barrier, sometimes referred to as ‘leaky’ gut (meaning inflammatory compounds can leak into the blood stream), and disruption of the levels of the gut’s microbial inhabitants, has been linked to almost every known health disorder. This includes digestive conditions, autoimmune disease, allergies, metabolic dysfunction, and mental health imbalances such as depression.13,14 Interestingly, turmeric has been shown to benefit many of these conditions.
The New Age Antidepressant
To isolate just one example, Australia’s very own psychologist and researcher Dr Adrian Lopresti, has published several impressive studies, finding the specific extract BCM-95™ Turmeric, when taken alone and in combination with the herb saffron, improves symptoms of major depression.15 There are multiple mechanisms to explain how it helps, but of most significance is its ability to reduce inflammation and increase protective compounds within brain regions that have been implicated in depression16,17 Yet again, it is not just the curcumin, but tumerones found within the whole herb that contribute to its antidepressant activity.18 While we’ve concluded that many of these actions are reliant on turmeric’s systemic tissue distribution, our assumptions may have been slightly misguided.
Exciting new evidence over the past decade has identified strong links between depression, changes in the microbiome, and a leaky gut; with inflammation thought to play the key intermediary role. Hence, reducing gut inflammation is a key therapeutic target for depression, and many other conditions as well. Conceivably, it is this mechanism through which turmeric works.
The Gut Loves Curry
Although the research is still in its infancy, studies suggest that the system-wide medicinal benefits of turmeric are, at least in part, mediated through its ability to correct both gut barrier integrity and microbiome disturbances – local gastrointestinal actions that are not reliant on its absorption (Figure 3). Turmeric interventions have been shown to increase the activity of genes which promote gut barrier healing, and offset the negative effects of drugs known to significantly damage the gut barrier.19 In addition to improving barrier integrity, turmeric targets the gut microbes, increasing their richness and diversity – markers of a healthy gut microbiome.20 The net effect is reduced inflammation within the gastrointestinal tract and throughout the entire body – producing body-wide health benefits. These combined actions may not render the question around turmeric absorption obsolete, but highlight the limitations of focusing on bioavailability alone. Simply put, turmeric extracts may not necessarily need high bioavailability to be a highly effective health remedy. So, how do you choose the right turmeric for you? Opt for extracts that produce the most impressive results when trialed in humans for the condition that you are taking turmeric for. For example, BCM-95™ is a great option for depression, and has also produced impressive results for osteoarthritis and rheumatoid arthritis. If you are not sure how to interpret clinical data yourself, speak to your naturopath or a Healthcare Practitioner who can. One thing we can predict with high probability, turmeric will continue to be trusted, loved and respected as a golden example of the benefits of natural therapies.
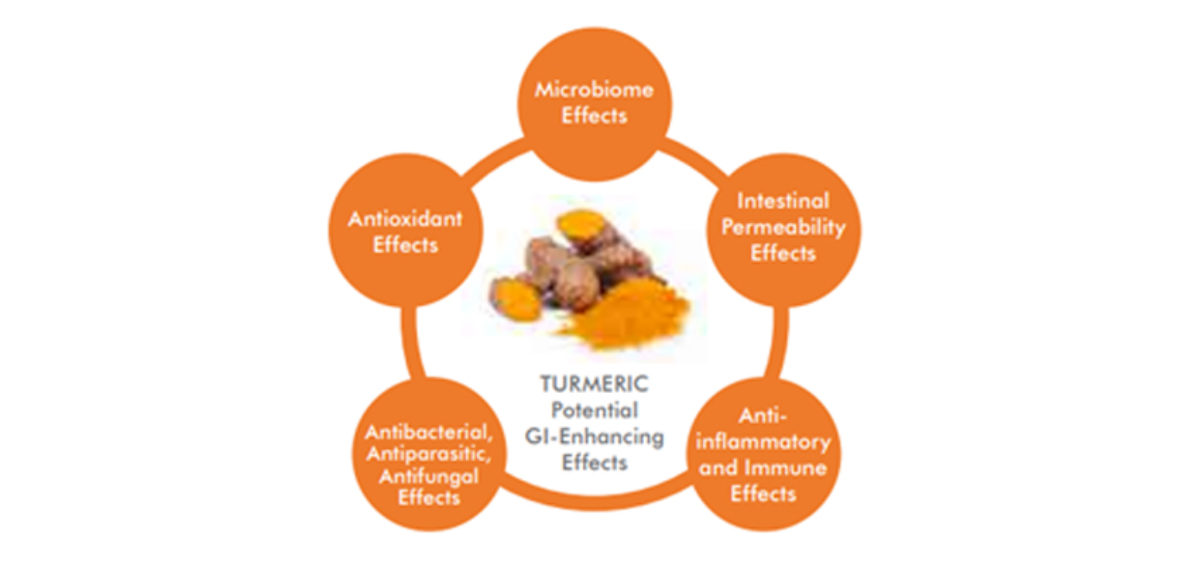
Figure 3: Potential Gastrointestinal-Enhancing Effects of Turmeric that May Contribute to its Systemic Health Effects.
References
1. Horayan A, Mukuchyan V, Mkrtchyan N, Minasyan N, Gasparvan S, Sargsyan A, et al. Efficacy and safety of curcumin and its combination with boswellic acid in osteoarthritis: a comparative randomised, double-blind, placebo-controlled study. BMC Complementary and Alternative Medicine. 2018;18(1)7. doi: 10.1186/s12906-017-2062-z.
2. Chandran B, Goel A. A randomized pilot study to assess the efficacy and safety of curcumin in patients with active rheumatoid arthritis. Phytotherapy Research. 2012 26(11): 1719-25.
3. Hewlings S, Kelman D. Curcumin: a review of it’s effect on human health. Foods. 2017 Oct 22;6(10). doi: 10.3390/foods6100092.
4. Mirmosayyeb O, Tanhaei A, Sohrabi HR, Martins RN, Tanhaei M, Najafi MA, et al. Possible Role of Common Spices as a Preventive and Therapeutic Agent for Alzheimer’s Disease. Int J Prev Med. 2017 Feb 7;8:5. doi: 10.4103/2008-7802.
5. Pulikkotil SJ, Nath S. Effects of curcumin on crevicular levels of IL-1β and CCL28 in experimental gingivitis. Aust Dent J. 2015 Sep;60(3):317-27
6. Natural Products Insider. 2016;6(14).
7. Del Prete D, Millan E, Pollastro F, Chianese G, Luciano P, Collado JA, et al. Turmeric Sesquiterpenoids: Expeditious Resolution, Comparative Bioactivity, and a New Bicyclic Turmeronoid. J Nat Prod. 2016 Feb 26;79(2):267-73. doi: 10.1021/acs.jnatprod.5b00637
8. Prasad S, Gupta SC, Tyagi AK, Aggarwal BB. Curcumin, a component of golden spice: from bedside to bench and back. Biotechnol Adv. 2014;32:1053–1064.
9. Tyagi AK, Prasad S, Yuan W, Li S, Aggarwal BB. Identification of a novel compound (β-sesquiphellandrene) from turmeric (Curcuma longa) with anticancer potential: comparison with curcumin. Invest New Drugs. 2015 Dec;33(6):1175-86.
10. Burgos-Morón E, Calderón-Montaño JM, Salvador J, Robles A, López-Lázaro M. The dark side of curcumin. Int J Cancer. 2010;126:1771-5
11. Prasad S, Gupta SC, Tyagi AK, Aggarwal BB. Curcumin, a component of golden spice: From bedside to bench and back. Biotechnol Adv. 2014;32:1053-64.
12. Helander HF, Fändriks L. Surface area of the digestive tract – revisited. Scandinavian Journal of Gastroenterology. 2014 Jun;49(6):681-9. doi: 10.3109/00365521.2014.898326.
13. Lloyd-Price J, Abu-Ali G, Huttenhower C. The healthy human microbiome. Genome Med. 2016;8:51.
14. Amalraj A, Pius A, Gopi S, Gopi S. Biological activities of curcuminoids, other biomolecules from turmeric and their derivatives – A review. J Tradit Complement Med. 2017 Apr;7(2):205–233.
15. Lopresti AL, Maes M, Maker GL, Hood SD, Drummond PD. Curcumin for the treatment of major depression: a randomised, double-blind, placebo controlled study. J Affect Disord. 2014;167:368-75.
16. Pereira Dias G, Cavegn N, Nix A, do Nascimento Bevilaqua M, Stangl D, Zainuddon M, et al. The Role of Dietary Polyphenols on Adult Hippocampal Neurogenesis: Molecular Mechanisms and Behavioural Effects on Depression and Anxiety. Oxid Med Cell Longev. 2012;2012:541971.
17. Xu Y, Ku B, Tie L, Yao H, Jiang W, Ma X, et al. Curcumin reverses the effects of chronic stress on behavior, the HPA axis, BDNF expression and phosphorylation of CREB. Brain Res. 2006 Nov 29;1122(1):56-64. Epub 2006 Oct 3.
18. Lopresti A. The Problem of Curcumin and Its Bioavailability: Could Its Gastrointestinal Influence Contribute to Its Overall Health-Enhancing Effects? Advances in Nutrition. 2018;9(1):41-50.
19. Lopresti A. The Problem of Curcumin and Its Bioavailability: Could Its Gastrointestinal Influence Contribute to Its Overall Health-Enhancing Effects? Advances in Nutrition. 2018;9(1):41-50.
20. Lopresti A. The Problem of Curcumin and Its Bioavailability: Could Its Gastrointestinal Influence Contribute to Its Overall Health-Enhancing Effects? Advances in Nutrition. 2018;9(1):41-50.
21. Adapted from: Lopresti A. The Problem of Curcumin and Its Bioavailability: Could Its Gastrointestinal Influence Contribute to Its Overall Health-Enhancing Effects? Advances in Nutrition. 2018;9(1):41-50
STRESS! A key factor in creating MENOPAUSE Symptoms.🤯 Time to put YOURSELF FIRST!🍃🙏💞

Menopause is a natural process where a woman transitions from her childbearing years to the next stage of her life. Whilst menopause usually occurs around age 50, a woman is said to be officially in menopause once she has not had a menstrual period for twelve consecutive months so this can occur at various ages. However, for many women, the months or years leading into menopause (known as perimenopause), can mark the onset of challenging symptoms including irregular menstrual cycles, flushing sensations, irritability and night sweats.
So what is actually happening within a woman’s body during menopause? Firstly, the ovaries stop producing hormones, particularly oestrogen, which results in the cessation of the menstrual period. You still need some oestrogen for important non-reproductive functions such as supporting bone health, therefore many other tissues including the brain, adrenal glands, and adipose (fat) tissue actually continue the role of oestrogen production for the remainder of a woman’s life, which begins to reveal why some woman experience menopause differently to others. What this means is – what impacts these tissues, impacts your symptoms.

Is it Getting Hot in Here or Is It Just Me?
Up to 80% of peri- and postmenopausal women report having vasomotor symptoms (VMS), such as hot flushes and night sweats; with up to half of these women reporting moderate or severe symptoms.1 The drop in oestrogen that naturally occurs in menopause is seen to be a significant culprit for hot flushes, however it is not the only cause. As similar levels of circulating oestrogen are found in women with and without VMS symptoms, this indicates other factors are at play.2
Remarkably, menopausal hot flushes are a result of the brains perception of temperature, due to the narrowing or reduction in something called the thermoneutral zone. Normal variations in body temperature within this zone means the body does not have to start shivering to warm up, or sweat to cool down. However, in menopause, the narrowing of this zone means that any slight elevation in temperature then triggers the sweating and flushing response, as the brain perceives the body’s temperature to be too hot.
As further proof of this, women experiencing menopausal flushes are not actually hotter in temperature than people not experiencing flushing – how fascinating!
Whilst declining oestrogen is one of the reasons for the narrowing of this zone, it is not the only cause. In fact, it is stress levels that play a larger role than oestrogen levels in triggering hot flushes. To highlight this, recent research has found that menopausal women have increased activity of the stress centre of the brain right before the onset of a hot flush.3
Therefore, it is vitally important to support a healthy stress response, not just hormones, to reduce menopausal symptoms.
Ingredients to Support Your Stress Response
The good news is that specific herbs and nutrients can support and nourish your stress response, and hence support your menopausal symptoms. Such ingredients include:
- B vitamins: as they have an increased demand during stressful times, with vitamins B5 and B6 especially required by your adrenal glands to synthesis their hormones. If a woman has a narrowed thermoneutral zone due to stress, and is hence experiencing VMS symptoms, B vitamins will help the adrenals function optimally.
- Magnesium: is a mineral that your body increases the elimination of when stressed, but is actually needed to calm the stress response. Therefore, supplying magnesium helps decrease your body’s sensitivity to stress, and as a bonus it helps improve energy levels. To learn more about the wonders of magnesium for hormonal conditions, read this blog.
- Rehmannia Six: a traditional Chinese medicine herbal combination that has been used for centuries to treat night sweats, anxiety and insomnia, making this an ideal formulation to discuss with your Practitioner for reducing symptoms associated with menopause. The influences of these herbs on the thermoneutral zone were demonstrated in a clinical trial on menopausal women, with the Rehmannia Six combination significantly reducing hot flushes and sweating.4
Time to Put Yourself First
Now you know that stress is a key factor creating menopause symptoms, it’s no surprise that your lifestyle plays a fundamental role in helping you sail through this life transition.
Research shows that mind-body therapies, such as yoga, tai chi, mindfulness, meditation, cognitive behavioral therapy and aerobic exercise improve overall menopausal symptoms, such as flushing, night sweats, insomnia and mood changes.5
Further, 65% of postmenopausal woman are classified as obese. Therefore, moving your body using the above methods will help to not only lose weight but also improve your symptoms, with evidence showing weight loss alone to be enough for some women to reduce their hot flushes.6
In this transitional time for women, it’s important to examine your stress levels, review your current lifestyle choices, and establish healthy habits. Remember, hormones are one part of the picture in menopause, but they aren’t the only contributor. Your whole body is made of many complexities, and addressing all aspects that influence your menopausal symptoms is vital when embarking on this next stage of life. For tailored support with your journey towards a balanced and vibrant body, click here to find your closest natural medicine Practitioner today.
References
1. Chiaramonte D, Ring M, Locke AB. Integrative Women’s Health. Med Clin North Am. 2017 Sep;101(5):955-975. doi: 10.1016/j.mcna.2017.04.010.
2. Freedman RR. Menopausal hot flashes: Mechanisms, endocrinology, treatment. J Steroid Biochem Mol Biol. 2014 Jul;142:115-20.
3. Diwadkar VA, Murphy ER, Freedman RR. Temporal sequencing of brain activations during naturally occurring thermoregulatory events. Cereb Cortex. 2014 Nov;24(11):3006-13. doi: 10.1093/cercor/bht155.
4. Zhang JP, Zhou DJ. Changes in leucocytic estrogen receptor levels in patients with climacteric syndrome and therapeutic effect of liuwei dihuang pills.Zhong Xi Yi Jie He Za Zhi. 1991 Sep;11(9):521-3,515. PMID: 1773463.
5. Goh VHH, Hart WG. Excess fat in the abdomen but not general obesity is associated with poorer metabolic and cardiovascular health in premenopausal and postmenopausal Asian women. Maturitas. 2018 Jan;107:33-38. doi: 10.1016/j.maturitas.2017.10.002
6. Thurston RC, Ewing LJ, Low CA, Christie AJ, Levine MD. Behavioral weight loss for the management of menopausal hot flashes: a pilot study. Menopause. 2015 Jan;22(1):59-65. doi: 10.1097/ GME. 0000000000000274.

 Is What You Heard About Turmeric True?
Is What You Heard About Turmeric True? 